Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
12 Dec
New Study: Acupuncture Shows Real Promise for Cancer ‘Brain Fog’
A new study finds acupuncture may help breast cancer survivors struggling with attention, memory and other cognitive problems.
11 Dec
Everyday Moves That Spike — or Reduce — Low Back Pain
Researchers look at how 10 common activities affect low back pain over the short and long term.
10 Dec
New Study Links Agent Orange to Rare Blood Cancer in Vietnam Vets
A landmark study finds Vietnam veterans exposed to Agent Orange face a significantly higher risk of developing myelodysplastic syndrome. Researchers hope this finding helps veterans get the health and disability benefits they’ve been denied for 50 years.
New Sunscreen Ingredient Could Soon Be Allowed in the U.S.
Americans may soon have access to a new sunscreen ingredient already used around the world.
The U.S. Food and Drug Administration (FDA) announced Dec. 11 that it is reviewing a proposal to allow bemotrizinol in sunscreens sold in the United States.
The ingredient is already approved and widely used in Europe, Australia and part...
- I. Edwards HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Many Older Americans Don’t See Themselves as Disabled, Survey Finds
Americans may be getting older and need help doing things that were once routine, but a new survey finds only a fraction of seniors see themselves as having a disability.
"It’s a familiar story," Megan Morris, director of the Disability Equity Collaborative at New York University, told KFF Health News. "Many people still fee...
- Carole Tanzer Miller HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
South Carolina Places 254 in Quarantine as Measles Cases Surge
South Carolina health officials say a measles outbreak is growing amid holiday travel and low vaccination rates, and they warn the spread could continue for weeks.
As of Dec. 10, the state’s Department of Public Health has confirmed 114 cases, nearly all in the state’s upstate region. Of 111 cases recorded there, 105 were in pe...
- I. Edwards HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
FDA Clears Home Brain-Stimulation Device to Help Treat Depression
An at-home device that sends a gentle electrical current to the brain to help treat depression has been cleared by the U.S. Food and Drug Administration (FDA).
Experts say the move could expand access to care for many folks.
The prescription headset, made by Sweden-based Flow Neuroscience, delivers low-level electrical stimulation to...
- I. Edwards HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Smokers Who Vape More Likely To Quit Or Cut Back, Study Argues
Smokers who use cigarettes and vape devices interchangeably might not be doing themselves as much of a disservice as once feared, a new study says.
These "dual users" are more likely to eventually quit smoking than people who smoke without vaping, researchers reported Dec. 10 in the journal Nicotine & Tobacco Research.
D...
- Dennis Thompson HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Virtual Nursing Doesn't Deliver, Hospital Nurses Say
Virtual nurses aren’t an effective way to help hospitals deal with a lack of staffing, a new study says.
Hospitals struggling to attract and retain nurses are trying out virtual nursing programs, in which nurses in remote locations rely on video and messaging technologies to keep tabs on patients, researchers said.
But these vi...
- Dennis Thompson HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Improved Bionic Hand Has A Mind Of Its Own, Researchers Say
The best way to improve amputees’ control over a bionic hand is to give the hand a mind of its own, a new study argues.
A bionic hand that’s controlled by an artificial intelligence (AI) program, but under the direction of the amputee, provides the best approximation of normal hand dexterity, researchers said Dec. 9 in the jour...
- Dennis Thompson HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
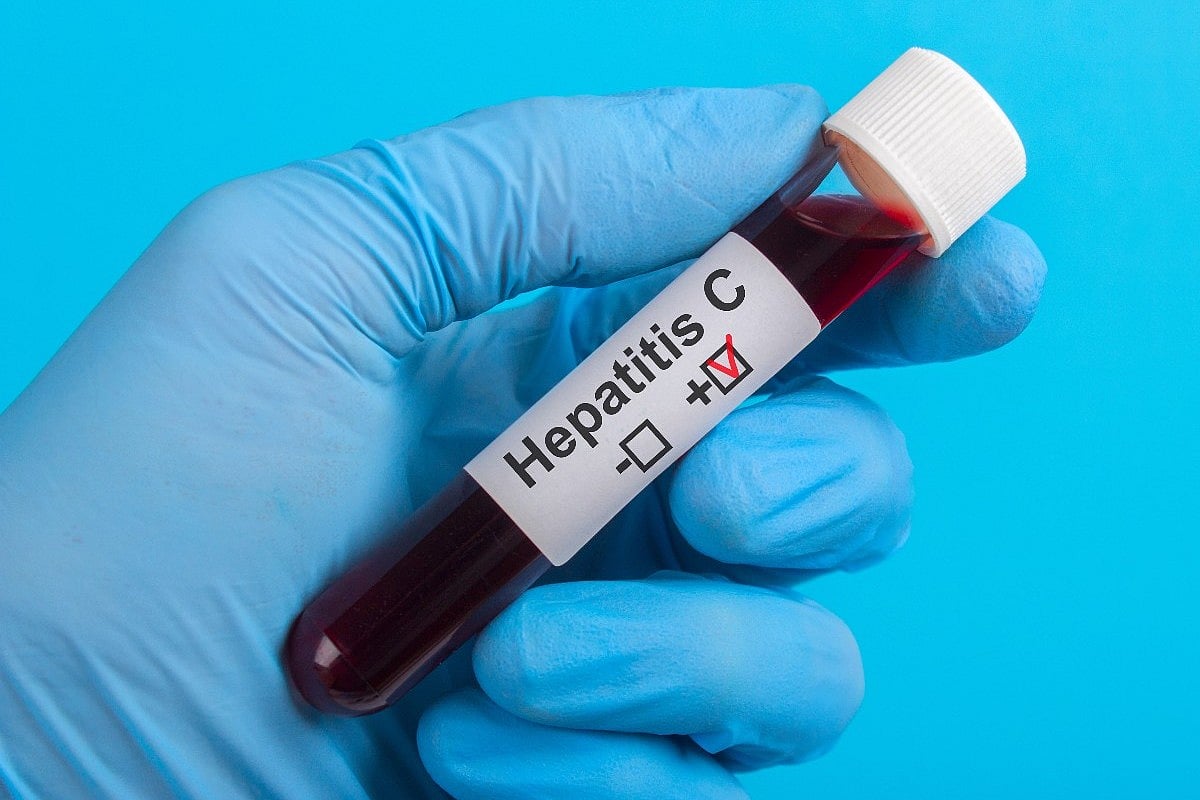
New 15-Minute Test For Hepatitis C Paves Way For Same-Day Treatment
People could learn within 15 minutes whether they are infected with hepatitis C, thanks to a rapid test developed by Northwestern University.
The test will allow doctors to diagnose infections during an office visit and kickstart patients’ treatment before they leave, researchers said.
“This test could revolutionize HCV c...
- Dennis Thompson HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Experimental Drug Provides Lasting Relief For Bleeding Condition
More than half of people with a rare life-threatening bleeding condition received lasting relief from an experimental antibody treatment, clinical trial results show.
Ianalumab, a monoclonal antibody, helped patients with immune thrombocytopenia (ITP) maintain safe platelet counts without serious bleeding episodes for at least a year, acco...
- Dennis Thompson HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Less Is More For Melanoma-Fighting Immunotherapy, Study Argues
Less might be more when it comes to immunotherapy treatment of melanoma, a new study says.
Lower doses of a drug used to treat melanoma can provide better results while reducing side effects, researchers reported Dec. 8 in the Journal of the National Cancer Institute.
“The results are highly interesting in oncology, as...
- Dennis Thompson HealthDay Reporter
- |
- December 12, 2025
- |
- Full Page
Suicide Deaths Fell Slightly in 2024, CDC Reports
The U.S. suicide rate dipped slightly in 2024, offering a small but hopeful improvement after years of increases, according to new provisional data from the U.S. Centers for Disease Control and Prevention (CDC).
A little over 48,800 people died by suicide last year, about 500 fewer than in 2023.
That translates to a national ra...
- I. Edwards HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
FDA Reviewing RSV Drugs for Infants, Though No Safety Issues Found
Federal regulators have begun a safety review of two RSV medicines used to protect infants, even though no safety problems have been reported.
The review covers Beyfortus (from Sanofi and AstraZeneca) and Enflonsia (from Merck), both monoclonal antibodies that help shield babies from respiratory syncytial virus, or RSV.
The mov...
- I. Edwards HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
Research Shows Imagining Positive Encounters Shapes Real-Life Feelings
Thinking about a positive moment with someone, even if it never happened, may actually make you like them more, new research shows.
A study published Dec. 10 in Nature Communications found that simply imagining a good interaction with a person can change your feelings toward them as well as how your brain stores informati...
- I. Edwards HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
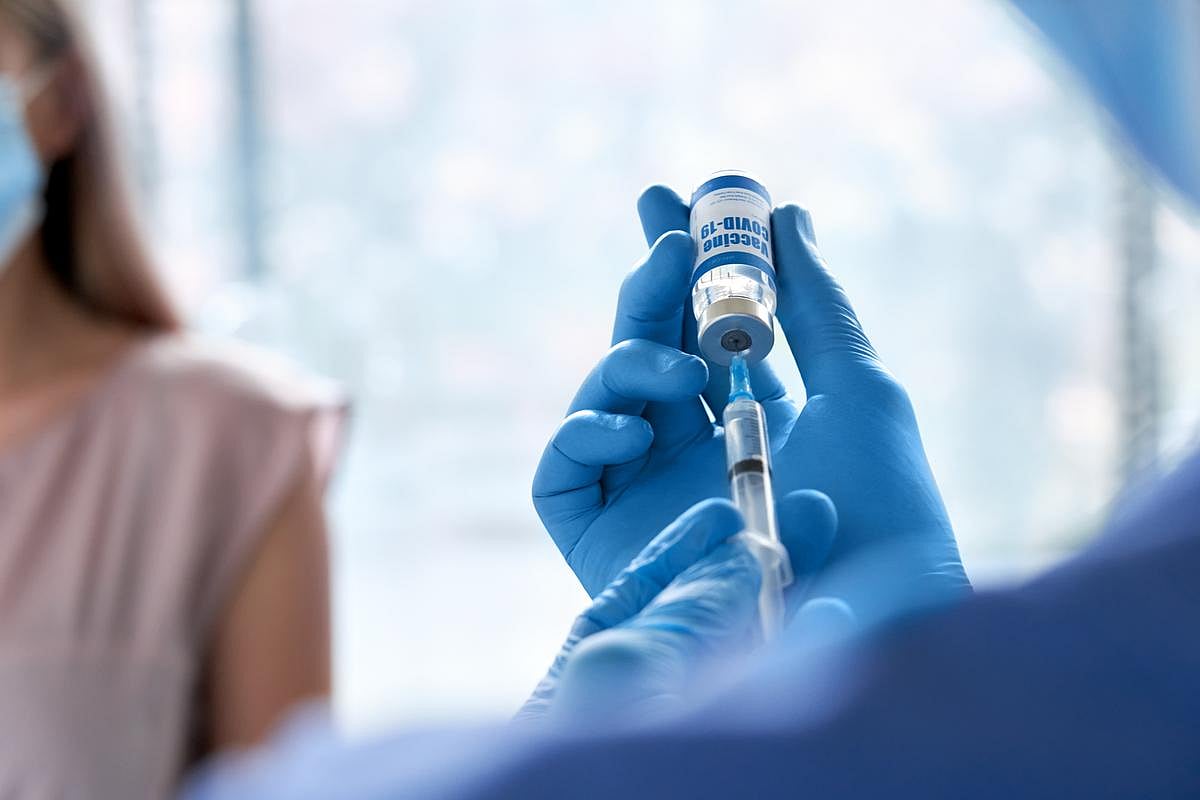
FDA Looks Into Reports of Deaths After COVID Vaccination
Federal officials say the U.S. Food and Drug Administration (FDA) is reviewing reports of possible deaths in adults and children following COVID-19 vaccination.
“FDA is doing a thorough investigation, across multiple age groups, of deaths potentially related to coronavirus vaccines,” said Andrew Nixon, spokesperson for the U.S....
- I. Edwards HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
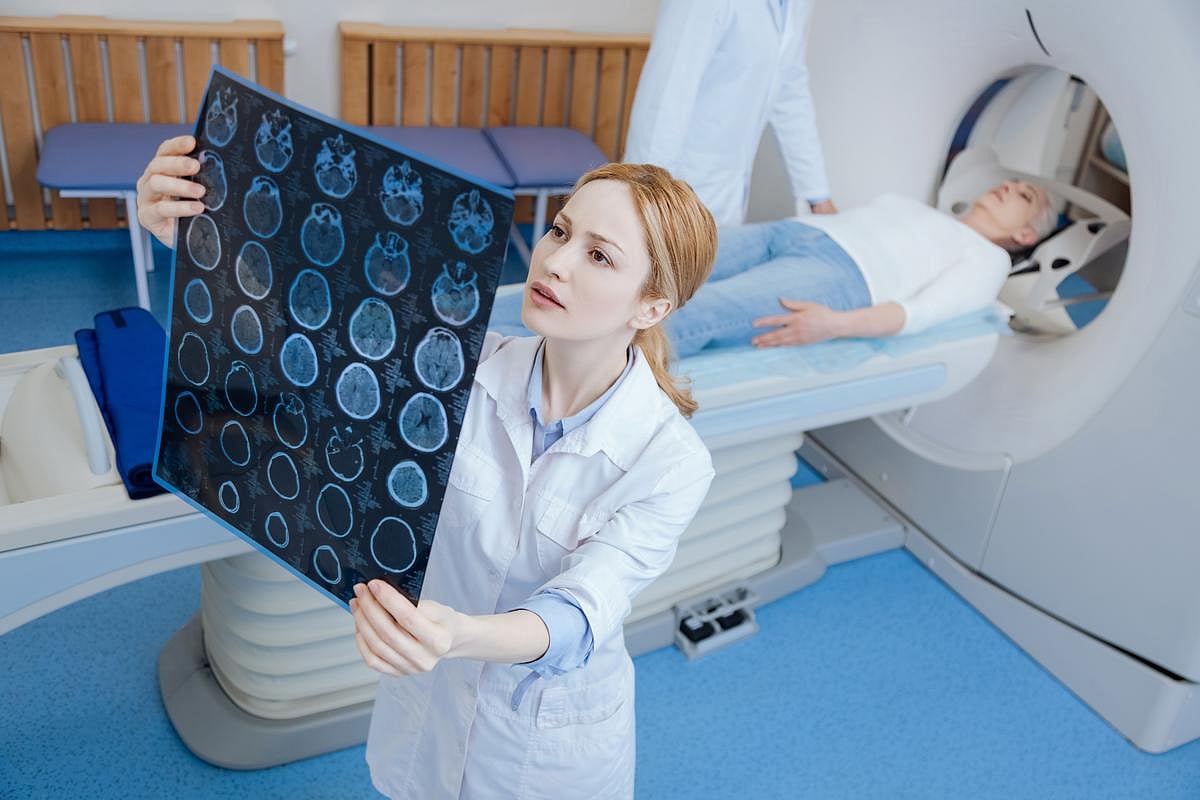
Medical Imaging Contributing To Water Pollution, Experts Say
Contrast chemicals injected into people for medical imaging scans are likely contributing to water pollution, a new study says.
Medicare patients alone received 13.5 billion milliliters of contrast media between 2011 and 2024, and those chemicals wound up in waterways after people excreted them, researchers recently reported in JAMA Ne...
- Dennis Thompson HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
Financial Toxicity Common Among Families Of Childhood Leukemia Patients
Childhood leukemia can land a family in dire financial straights, a new study says.
Nearly a third of families develop serious financial difficulties while their child receives chemotherapy for acute lymphoblastic leukemia (ALL), the most common childhood cancer, researchers reported Sunday at a meeting of the American Society of Hematolog...
- Dennis Thompson HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
Leukemia Strikes Black Patients Earlier, With Higher Risk Of Death, Study Says
Leukemia poses a considerably higher risk to Black patients compared to white patients, a new study says.
Black patients are diagnosed with acute myeloid leukemia at a younger age and are more likely to die from the blood cancer, according to findings presented Saturday at a meeting of the American Society of Hematology in Orlando.
&...
- Dennis Thompson HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
Social Media Draining Kids' Ability To Concentrate, Study Argues
Social media could be draining children of their ability to concentrate, a new study says.
Children who spend a lot of time on Instagram, Snapchat, TikTok, Facebook, Twitter or Messenger gradually become less able to focus and pay attention, researchers reported Dec. 8 in the journal Pediatrics Open Science.
This might parti...
- Dennis Thompson HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
Parents Might Pass Depression Down To Kids Through One Specific Symptom, Experts Say
Children of depressed parents are more likely to develop depression themselves, and a new study suggests this risk might be tied to one specific symptom of depression.
It’s already known that depression in parents can affect how children’s brains respond to positive and negative feedback, researchers said.
That might be d...
- Dennis Thompson HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page
Nerve Blocks Now Recommended For ER Migraine Treatment
People hospitalized for a debilitating migraine should receive targeted nerve blocks rather than IV opioids to quell their pain, according to a major update of treatment guidelines.
Doctors should use a nerve block injection to stop pain signals from thrumming through the occipital nerves located near the top of the spine, a report publish...
- Dennis Thompson HealthDay Reporter
- |
- December 11, 2025
- |
- Full Page