Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
19 Jan
Major Evidence Review Finds No Link Between Tylenol During Pregnancy and Autism or ADHD
A review of 43 high-quality studies involving hundreds of thousands of children finds no evidence that taking acetaminophen during pregnancy increases a child’s risk for autism, ADHD or intellectual disability.
16 Jan
Early Exposure to Air Pollution May Raise Childhood Blood Pressure
A new study finds children exposed to fine particulate matter during pregnancy and early childhood are more likely to have higher blood pressure from ages 5 to 12.
15 Jan
Is No Social Media as Risky as Too Much for Teens?
A new study finds both heavy use and zero use of social media can negatively impact teen well-being.
As Forests Shrink, Mosquitoes Are Turning to Humans for Blood
As people cut deeper into Brazil’s Atlantic Forest, mosquitoes may be changing who they bite, and a new study suggests they have a new favorite target: humans.
The Atlantic Forest once stretched across much of Brazil’s coast and was home to hundreds of animal species. Today, only about one-third of the forest remains, largely d...
- I. Edwards HealthDay Reporter
- |
- January 19, 2026
- |
- Full Page
New Coffee Chemicals Show Promise for Managing Type 2 Diabetes
Coffee may do more than boost energy.
New research suggests that certain compounds found in roasted coffee beans could help slow how quickly sugar enters the bloodstream, a finding that could one day support new foods aimed at managing type 2 diabetes.
Scientists have identified three previously unknown compounds in roasted coffee th...
- I. Edwards HealthDay Reporter
- |
- January 19, 2026
- |
- Full Page
Why Connecting With Others is Good For Your Health
A third of U.S. adults are lonely, and a quarter lack social and emotional support — and research underscores that’s just not healthy.
"Humans are a social species. We are highly dependent on others from birth," said Elizabeth Necka, an expert on social and behavioral science at the National Institutes of Health. "So feeling so...
- Carole Tanzer Miller HealthDay Reporter
- |
- January 18, 2026
- |
- Full Page
What You Can Do To Prevent Chronic Kidney Disease
More than 14% of U.S. adults have some level of chronic kidney disease — and most have no idea.
"People with chronic kidney disease generally have no symptoms until they’re very near kidney failure," said kidney-health researcher Dr. Michael Shlipak of the University of California, San Francisco.
Chronic kidney dise...
- Carole Tanzer Miller HealthDay Reporter
- |
- January 17, 2026
- |
- Full Page
Popular Super Greens Supplement Recalled After Salmonella Illnesses Reported
A powdered super greens supplement sold across the U.S. has been recalled after federal health officials linked it to a Salmonella outbreak that has sickened people in at least 21 states.
At least 45 people have become ill after consuming Live it Up-brand Super Greens powder, according to U.S. Food and Drug Administration (FDA) an...
- I. Edwards HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Mistrust Fuels Drop in Deceased Organ Donations, Kidney Transplants
More than 100,000 people in the U.S. are waiting for an organ transplant, and most need a kidney. Thousands die each year before a matching organ becomes available.
New federal data reviewed by the Kidney Transplant Collaborative show that 116 fewer kidney transplants were performed last year than in 2024.
While that difference...
- I. Edwards HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Trump Administration Restores Nearly $2 Billion in Mental Health Grants
Federal funding for mental health and addiction treatment programs will continue after the Trump administration abruptly reversed a plan to end nearly $2 billion in grants across the country.
Late Tuesday, thousands of grants overseen by Substance Abuse and Mental Health Services Administration (SAMHSA) were suddenly terminated.
<...- I. Edwards HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Whole Milk Returns to School Lunches
Whole milk may soon be back on school lunch trays across the U.S.
President Donald Trump signed a new law Wednesday that allows schools to serve whole and 2% milk again, reversing rules that limited higher-fat milk options for more than a decade.
The law, called the Whole Milk for Healthy Kids Act, lets schools in the National School...
- I. Edwards HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Nerve Stimulation Halts Depression In More Than 20% Of Patients, Clinical Trial Reports
Treatment-resistant depression might be eased using an implant that sends electrical pulses to one of the body’s major nerve clusters, a new study says.
The implant, placed under the skin in the chest, sends carefully calibrated electrical pulses to the left vagus nerve — a major conduit between the brain and internal organs.
- Dennis Thompson HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
'If In Doubt, Sit Them Out,' Insists New Concussion Guidance For Parents
The bottom line for managing youth sports concussions is “if in doubt, sit them out,” new guidelines say.
Earlier recognition of a concussion — and removal from play — will help a young athlete more quickly recover and return to competition, according to an easy-to-follow guide published recently in the Archives...
- Dennis Thompson HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Air Pollution Increases Risk of Childhood High Blood Pressure
Children might wind up with high blood pressure due to air pollution exposure that occurred in the womb or the cradle, a new study says.
Exposure to smog before and after birth increases a child’s odds of having higher blood pressure between ages 5 and 12, researchers report in the March 2026 issue of the journal Environmental Re...
- Dennis Thompson HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Medical Students Not Being Adequately Trained To Confront Death, Review Finds
Doctors encounter death more than people in nearly all other lines of work.
That’s the price they pay for a career spent saving lives and helping people.
But modern medical education leaves doctors little-prepared for this inevitable challenge, a new evidence review says.
There’s minimal evidence-based education ava...
- Dennis Thompson HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Fingertip Blood Oxygen Monitors Are Less Accurate For People Of Color, Study Finds
Most everyone’s seen one in a doctor’s office or hospital room — the finger clip device that reads a person’s pulse and blood oxygen levels.
But new research shows these ubiquitous devices appear to give misleading readings for people with darker skin tones, potentially affecting their care.
Pulse oximeters gi...
- Dennis Thompson HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
Drunk For No Reason? Could Be A Rare Gut Disorder, Researchers Say
Ever felt drunk, hammered, wasted, absolutely smashed — but you haven’t touched a drop of alcohol?
You might have suffered from a rare gut condition called auto-brewery syndrome, which causes alcohol intoxication in people who haven’t had anything to drink.
Researchers now think they’ve figured out the specifi...
- Dennis Thompson HealthDay Reporter
- |
- January 16, 2026
- |
- Full Page
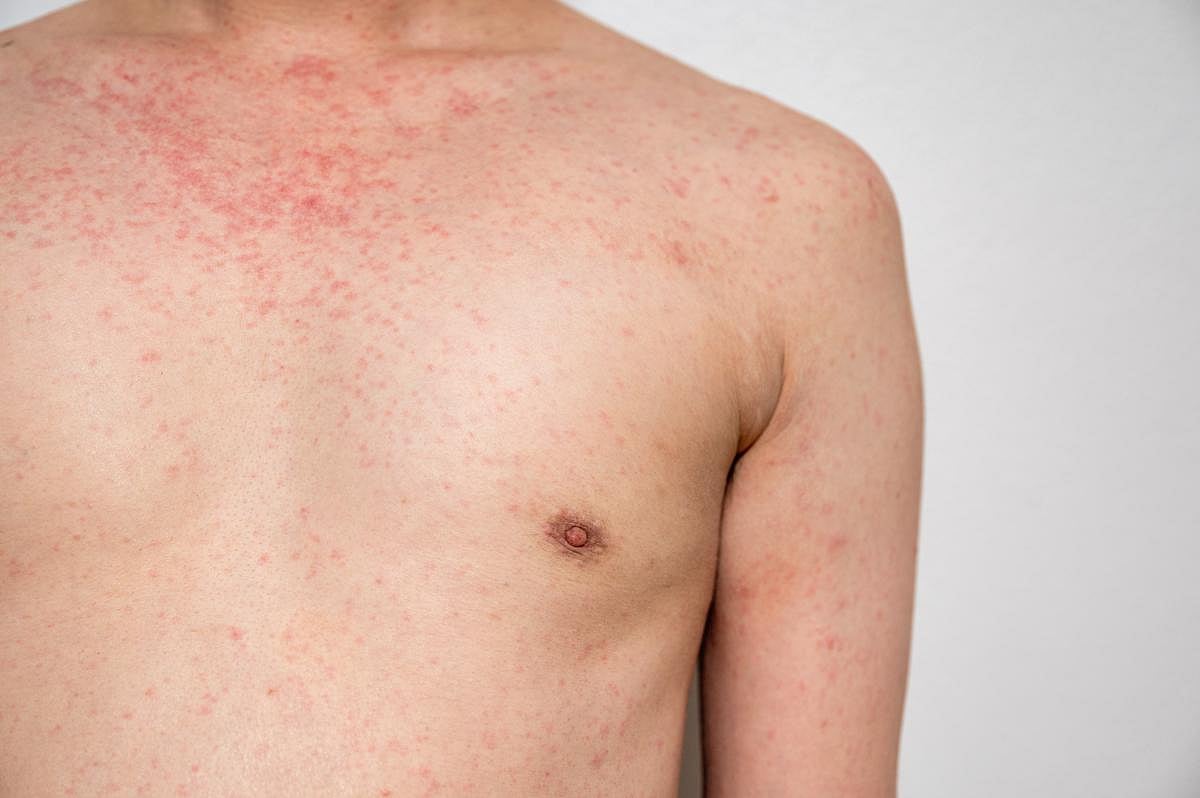
Measles Outbreaks Grow in South Carolina and Southwest, Officials Warn
Health officials are struggling to contain two growing measles outbreaks in the U.S., as new cases continue to climb weeks after holiday travel and gatherings helped the virus spread.
In South Carolina, officials confirmed 124 new measles cases since Friday, pushing the state’s total to 434 cases as of Tuesday.
The outbre...
- I. Edwards HealthDay Reporter
- |
- January 15, 2026
- |
- Full Page
Small Daily Habit Changes Could Add Years to Your Life, Study Finds
You don’t need a new diet plan or a gym membership to improve your health in 2026.
New research suggests that very small daily changes like sleeping a few extra minutes, moving a little more and eating slightly better may help people live longer and stay healthier as they age.
University of Sydney researchers studied more...
- I. Edwards HealthDay Reporter
- |
- January 15, 2026
- |
- Full Page
Obamacare Enrollment Drops After Premium Subsidies Expire
Fewer Americans are signing up for Obamacare this year after extra financial help that lowered monthly premiums expired, new counts show.
As of early January, 22.8 million people had enrolled in Affordable Care Act (ACA) health plans for coverage starting Jan. 1. That’s down from 24.2 million people who were enrolled by the end of la...
- I. Edwards HealthDay Reporter
- |
- January 15, 2026
- |
- Full Page
FDA Moves To Remove Suicide Warnings From GLP-1 Weight Loss Drugs
Federal health regulators say popular weight loss drugs like Wegovy and Zepbound do not increase the risk of suicidal thoughts, and they have asked drugmakers to remove those warnings from medication labels.
The U.S. Food and Drug Administration (FDA) said Tuesday that its latest safety review found no link between GLP-1 weight loss drugs ...
- I. Edwards HealthDay Reporter
- |
- January 15, 2026
- |
- Full Page
Burn Pits Loaded Veterans' Lungs With Carbon, Study Says
Exposure to open-air burn pits during post-9/11 military conflicts in Iraq and Afghanistan likely caused lung damage in some U.S. veterans, a new study says.
Veterans with deployment-related lung disease had higher levels of carbon-based particles in their lungs compared to healthy controls, researchers recently wrote in the journal Sc...
- Dennis Thompson HealthDay Reporter
- |
- January 15, 2026
- |
- Full Page
Can Teens Use Social Media Too Little For Their Own Good? Maybe, Study Says
There appears to be a “Goldilocks zone” when it comes to social media use among teenagers.
Too much social media use can negatively affect a teenager’s well-being, a new study finds, dovetailing with results of previous research.
But too little social media use also can have a bad impact on well-being, researchers r...
- Dennis Thompson HealthDay Reporter
- |
- January 15, 2026
- |
- Full Page