Get Healthy!
Staying informed is also a great way to stay healthy. Keep up-to-date with all the latest health news here.
10 Jul
Severe Withdrawal From Antidepressants Uncommon, Study Finds
A review of 50 clinical trials on antidepressants and withdrawal concludes most patients experience one additional symptom, the most common being dizziness and nausea.
09 Jul
A Usually “Harmless Virus” May Trigger or Contribute to Parkinson’s Disease
A new study out of Northwestern Medicine finds evidence of the human pegivirus in the brains of people with Parkinson’s disease, but not in the brains of people without the neurological condition.
08 Jul
How Does BMI Affect Breast Cancer Risk in Postmenopausal Women?
A new study finds the combination of excess weight and heart disease in postmenopausal women is associated with an especially high risk of developing breast cancer.
Life Expectancy in California Has Not Recovered From COVID Drop
Even four years after the start of the COVID-19 pandemic, California residents aren’t living as long as they used to.
New research published July 9 in the Journal of the American Medical Association shows that though the state’s life expectancy is improving, it hasn’t returned to pre-pandemic levels. In 2024, the...
- I. Edwards HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Susan Monarez Advances in Process to Lead CDC
Susan Monarez is one step closer to becoming the next director of the U.S. Centers for Disease Control and Prevention (CDC).
On Wednesday, the U.S. Senate’s health committee voted 12-11 to move her nomination forward. The vote was along party lines, with all Democrats voting no, The Associated Press reported.
If confir...
- I. Edwards HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Experts Say There’s No Safe Amount of Processed Meat
A new study finds that eating even a little processed meat, drinking soda or consuming trans fats puts you at risk for serious health problems.
The research, published recently in the journal Nature Medicine, looked at more than 60 earlier studies on how diet affects the risk of type 2 diabetes, colon cancer and heart disease.&nbs...
- I. Edwards HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Lyme Disease Patients Aren't Getting Proper Follow-Up Care
Most folks diagnosed with Lyme disease aren’t getting the follow-up care they need, a new study says.
Only one-third of people (35%) with ongoing early-stage Lyme disease symptoms checked back in with their doctor, researchers reported today in the journal Frontiers in Medicine.
Further, evidence shows the U.S. Centers...
- Dennis Thompson HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
'Old' Brains Increase Risk Of Death, Alzheimer's
They say age is all in your mind — and that might literally be true, a new study reveals.
People with “young” brains — brains aging more slowly than their actual age — are much less likely to die or develop Alzheimer’s disease than those with “old” brains suffering from accelerated aging, res...
- Dennis Thompson HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Air Pollution Linked To Common Brain Tumors
Folks who breathe in more air pollution have a higher risk of developing a common non-cancerous brain tumor, a new study says.
Several different types of air pollutants, including particle pollution and nitrogen dioxide, appear to increase risk of meningiomas — tumors that form in the layers of tissue that cover the brain and spinal ...
- Dennis Thompson HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Lead Exposure Can Harm Kids' Memory, Study Says
Even low levels of lead exposure can harm kids' working memory, potentially affecting their education and development, according to a new study.
Exposure to lead in the womb or during early childhood appears to increase kids' risk of memory decay, accelerating the rate at which they forget information, researchers reported July 9 in the jo...
- Dennis Thompson HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Loneliness Preys On Mental, Physical Health
Loneliness dramatically increases a person’s risk of depression and poor health, a new study says.
Half of folks who say they always feel lonely (50%) have clinical depression, compared with just 10% of those who report never feeling lonely, researchers reported July 9 in the journal PLOS One.
They also have many more ...
- Dennis Thompson HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Trying to Quit Smoking? These Expert-Backed Tips Can Help
According to the U.S. Centers for Disease Control and Prevention (CDC), in 2022, the majority of the 28.8 million U.S. adults who smoked cigarettes wanted to quit; approximately half had tried to quit, but fewer than 10% were successful.
Many folks say quitting smoking was the hardest thing they have ever done. This includes pe...
- David Hill, MD, Chair, Board of Directors, American Lung Association HealthDay Reporter
- |
- July 10, 2025
- |
- Full Page
Barbie's Latest Look? It Includes an Insulin Pump and Glucose Monitor
Barbie’s latest look includes a polka-dot crop top, chunky heels — and an insulin pump.
Mattel has released its first-ever Barbie with type 1 diabetes, complete with a glucose monitor, phone app and a purse packed with supplies. The goal? To help kids with diabetes feel seen — and to show that managing a health condition ...
- I. Edwards HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
RFK Jr. Praises Meal Program Critics Say Is Ultra-Processed
A government-backed meal delivery service for people on Medicaid and Medicare is getting national attention — but not all of it is positive.
Health Secretary Robert F. Kennedy Jr. recently praised Mom’s Meals, a company that sends prepackaged meals to people who are older or living with illnesses like cancer or diabetes, Th...
- I. Edwards HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
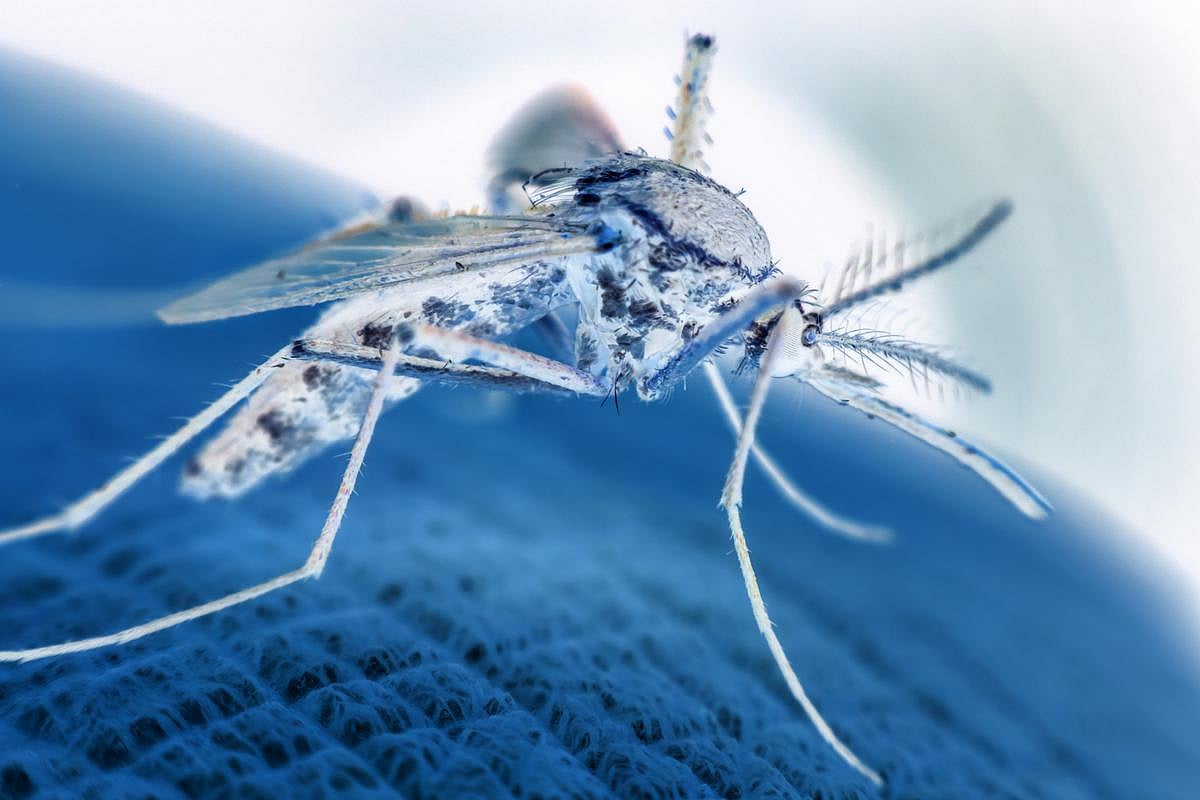
First Malaria Drug Approved for Newborns and Small Babies
A new malaria treatment has been approved for newborns and infants under 11 pounds, filling a major gap in care for some of the most vulnerable children.
The medicine, called Coartem Baby (also known as Riamet Baby), was approved by Switzerland’s health agency, Swissmedic, The Washington Post reported.
It was dev...
- I. Edwards HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
Fruits And Veggies Protective Against IBD, Study Says
A healthy plant-based diet might protect people from inflammatory bowel diseases, a new study says.
People noshing healthy plant-based foods had a 14% lower risk of Crohn’s disease and an 8% lower risk of ulcerative colitis, researchers found.
On the other hand, an unhealthy diet containing more animal fats and vegetable oils w...
- Dennis Thompson HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
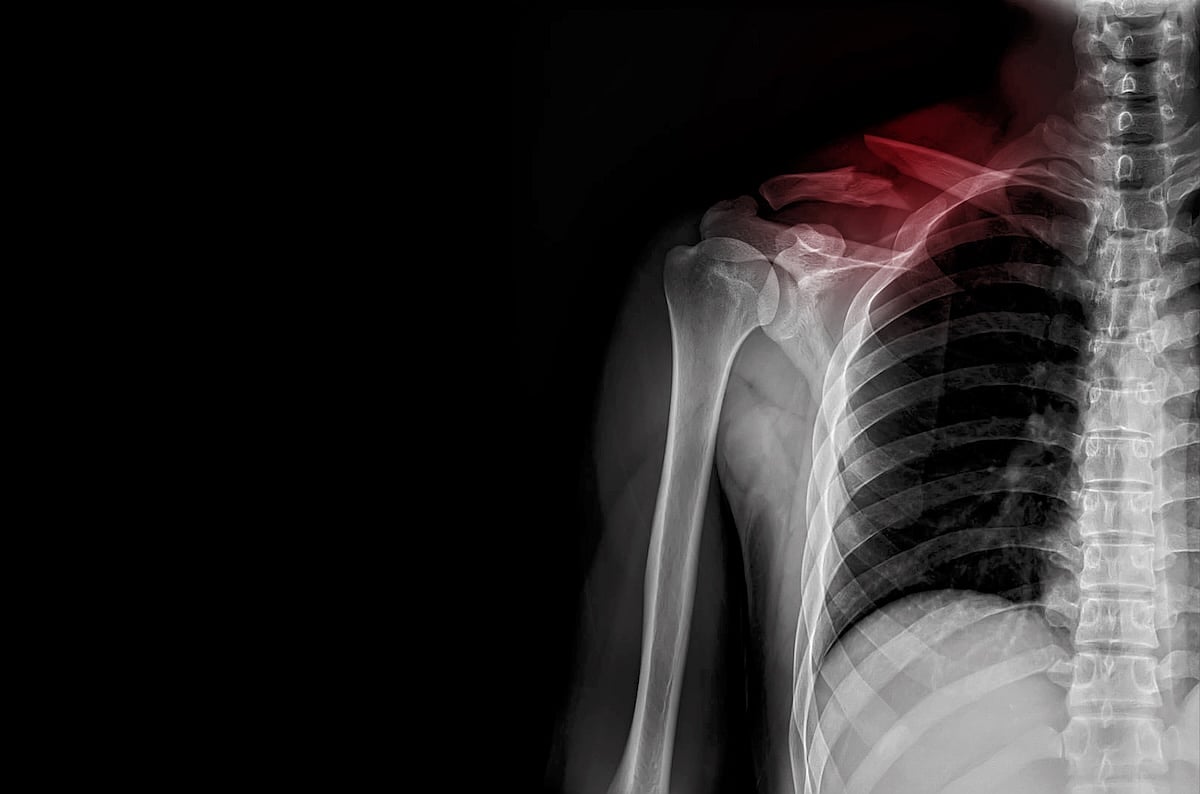
Broken Collarbone Hospitalizations Increase Among Children
More kids are being hospitalized for broken collarbones, a new study has found.
In fact, the hospitalization rate for broken collarbones more than doubled among children between 2014 and 2021, researchers reported.
This increase occurred even though the overall rate of childhood clavicle fractures remained relatively stable during th...
- Dennis Thompson HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
AI Displays Racial Bias Evaluating Mental Health Cases
AI programs can exhibit racial bias when evaluating patients for mental health problems, a new study says.
Psychiatric recommendations from four large language models (LLMs) changed when a patient’s record noted they were African American, researchers recently reported in the journal NPJ Digital Medicine.
“Most o...
- Dennis Thompson HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
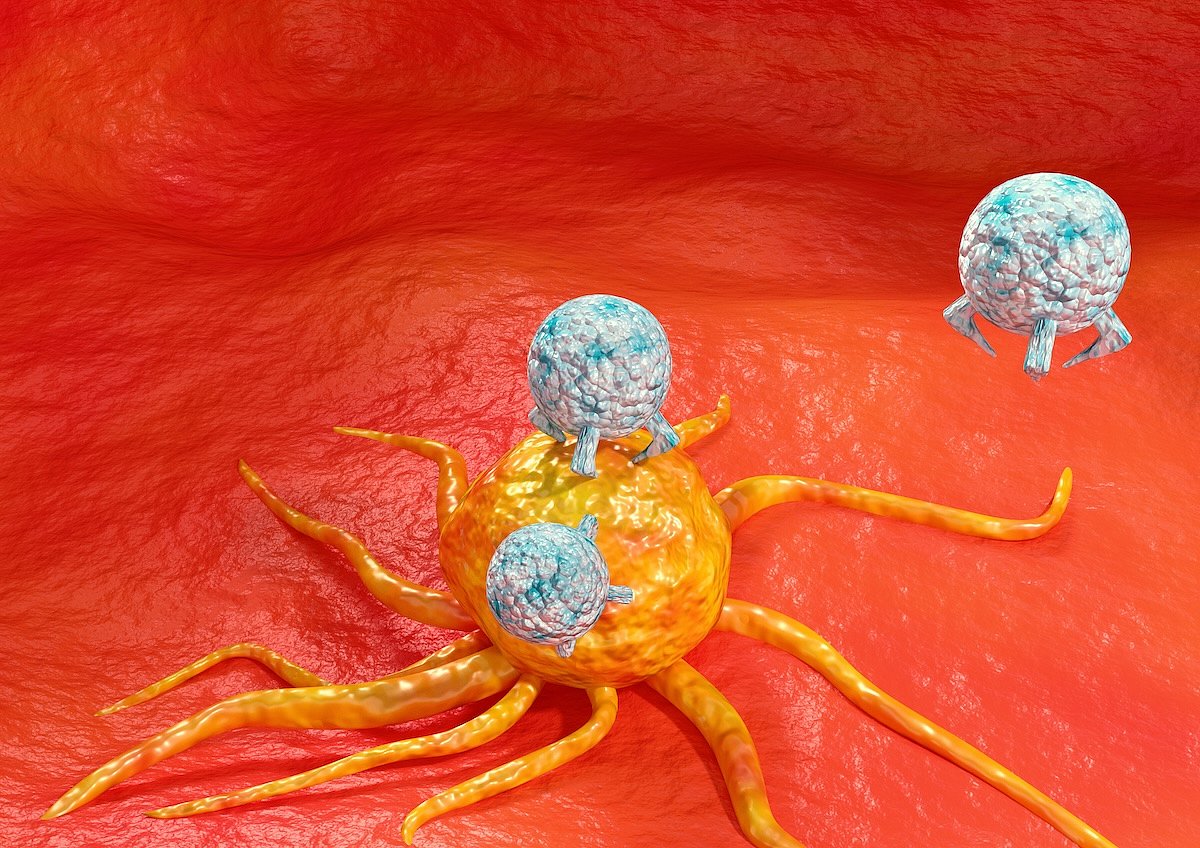
Insured? You're More Likely To Survive Cancer Through Immunotherapy Treatment
Powerful new immunotherapies are offering fresh hope for patients with many different types of cancer.
Unfortunately, that hope doesn’t extend to people without health insurance, a new study says.
Immune checkpoint inhibitors (ICIs) are revolutionizing cancer treatment by helping the immune system better find and attack cancer ...
- Dennis Thompson HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
Optimistic? Your Asthma Might Improve, Study Says
Want your asthma to improve? Cultivate a positive outlook, researchers say.
An asthma patient’s level of optimism or pessimism can influence how their symptoms progress, a new study says.
People who expect their asthma and health to get worse wind up reporting more symptoms over time, researchers reported recently in the journa...
- Dennis Thompson HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
'Harmless' Virus Might Trigger Parkinson's Disease, Researchers Say
A common virus once thought harmless to humans might be linked to Parkinson’s disease, a new study says.
The germ, Human Pegivirus (HPgV), was found in half the autopsied brains of patients with Parkinson’s, but not in any brains from healthy people, researchers reported July 8 in the journal JCI Insight.
“...
- Dennis Thompson HealthDay Reporter
- |
- July 9, 2025
- |
- Full Page
These Items Sold at Costco Have Been Recalled — Check Your Home
If you shop at Costco, you may want to check your home for items that have recently been recalled.
In the past few months, the retailer has flagged nearly a dozen products due to safety or health risks.
Some were sold directly in Costco stores, while others were purchased through Costco Next, a program that lets shoppers buy items st...
- I. Edwards HealthDay Reporter
- |
- July 8, 2025
- |
- Full Page
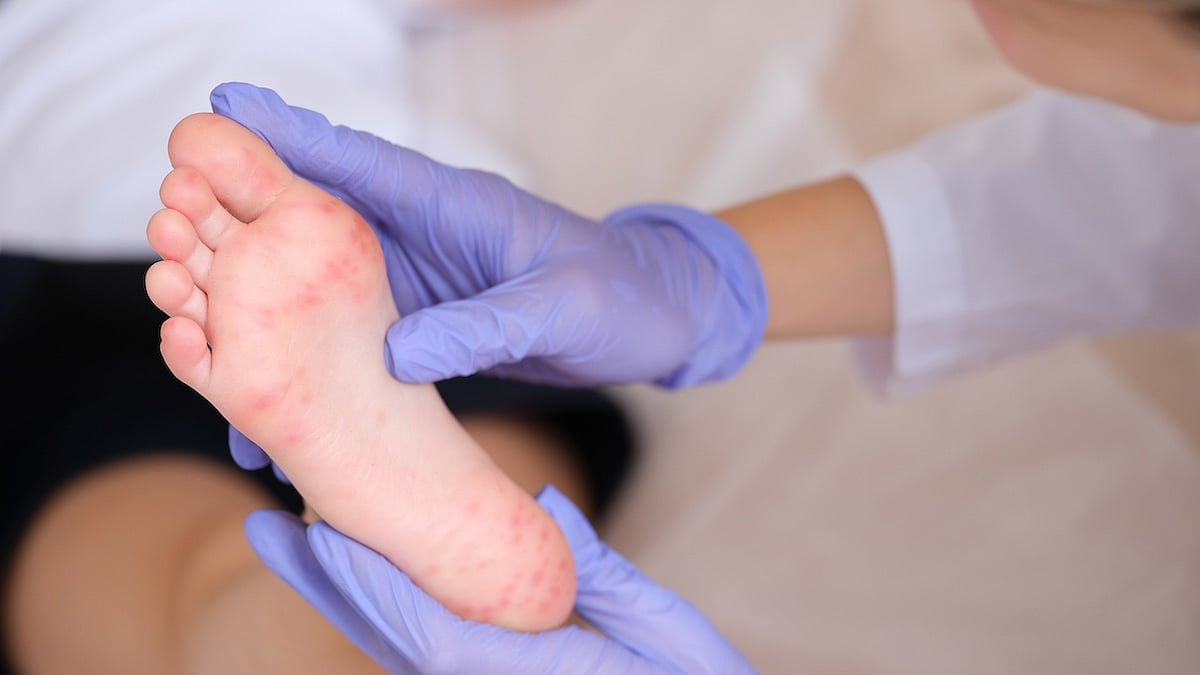
U.S. Measles Cases Hit Highest Level Since Disease Was Eliminated in 2000
Measles cases in the United States have reached their highest level in 25 years, with more than 1,270 confirmed cases this year.
That number surpasses the last record of 1,274 cases set in 2019, according to new data from Johns Hopkins University.
Experts suspect the true number may be much higher, since many cases go unreported. So ...
- I. Edwards HealthDay Reporter
- |
- July 8, 2025
- |
- Full Page