Manténgase sano!
Mantenerse informado(a) promueve la buena salud. Manténgase al día con las últimas noticias médicas encontradas aquí.
02 Apr
Occasional Heavy Drinking May Triple Risk of Liver Damage, Study Finds
New research finds even occasional heavy drinking — just once a month — may raise the risk of serious liver scarring, even in otherwise moderate drinkers.
01 Apr
Study Questions Effectiveness of KT Tape for Pain Relief
A large review of more than 300 studies finds KT tape may offer short-term pain relief, but its overall benefits remain uncertain. Researchers say it shows little impact on strength, mobility, or long-term outcomes.
31 Mar
Alternative Therapies Linked to Lower Breast Cancer Survival, Study Finds
New research suggests breast cancer patients who choose to fight their disease with complementary or alternative therapies are nearly 4 times more likely to die within 5 years.
FDA Recalls Wawa Milk Over Possible Plastic Contamination
Milk sold at convenience stores in four states is being recalled amid concerns about possible plastic contamination.
The U.S. Food and Drug Administration (FDA) said the recall affects 16-ounce plastic bottles of Wawa milk sold in Delaware, Maryland, New Jersey and Pennsylvania.
The issue was discovered after "foreign plastic materia...
- HealthDay Staff HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
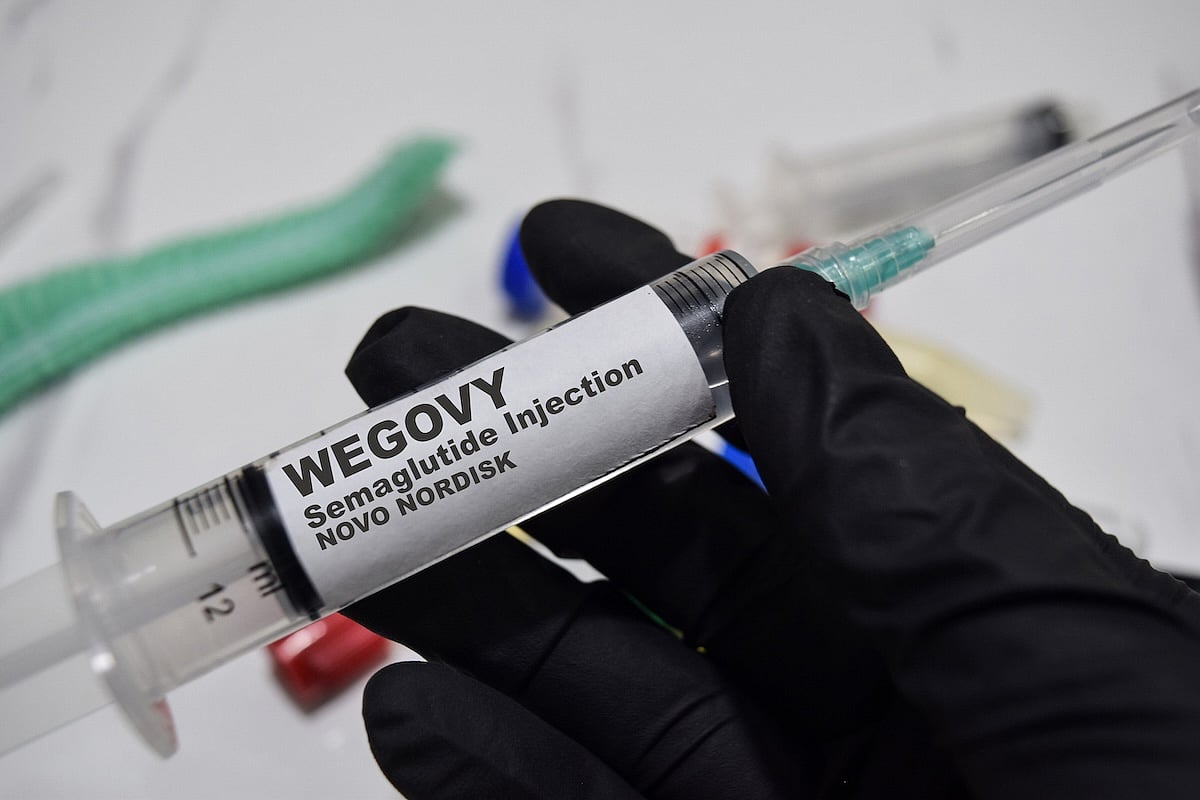
Wegovy Maker Launches Lower-Cost Subscription Plans
A popular weight loss drug may soon be more affordable for some people.
Danish pharmaceutical company Novo Nordisk has launched a subscription program for its obesity treatment Wegovy, offering lower and more predictable monthly prices.
The program is aimed at those who pay for the medication themselves, The Wall Street Journal
- HealthDay Staff HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
FDA Approves New Weight Loss Pill in Record Time
A new daily pill to help with weight loss has been approved by the U.S. Food and Drug Administration (FDA), and it moved through review faster than most drugs in recent years.
The drug, called Foundayo and developed for Eli Lilly, was approved in just 50 days. That’s 294 days ahead of schedule.
It is the fastest approval of a n...
- HealthDay Staff HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
Lawsuit Over Viral David Protein Bars Dropped Without Explanation
A lawsuit claiming popular protein bars had misleading nutrition labels has been dropped, but questions about the bars remain.
The case targeted David bars, which have gained a massive amount of attention online, especially among health and wellness influencers.
Filed in January, the lawsuit claimed independent lab tests showed the b...
- HealthDay Staff HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
Pandemic Spurred Increase In Screen Time Among Children, Teens
The COVID-19 pandemic fueled a dramatic rise in screen use among children and teenagers, a new evidence review says.
Kids spent more time with screens after the pandemic, using computers, video games, smartphones and tablets at rates higher than before COVID struck, researchers recently reported in the journal Clinical Child Psychology...
- Dennis Thompson HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
Siblings Crucial To Middle-Aged People Grieving The Loss Of A Parent, Study Says
Having more brothers and sisters might make it easier for middle-aged folks to cope with the death of a parent, especially a mother, a new study says.
Middle-aged adults needed fewer antidepressants and other mental health drugs before and after a parent’s death if they were supported by a network of siblings, researchers reported Ma...
- Dennis Thompson HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
New Rapid Urine Test Could Revolutionize Treatment of UTIs
A new rapid urine test could lead to more targeted and effective treatment of urinary tract infections (UTI), researchers say.
It currently takes labs two to three days to determine which antibiotic would work best against an individual’s UTI.
But the new test can turn around results in just under six hours, creating the potent...
- Dennis Thompson HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
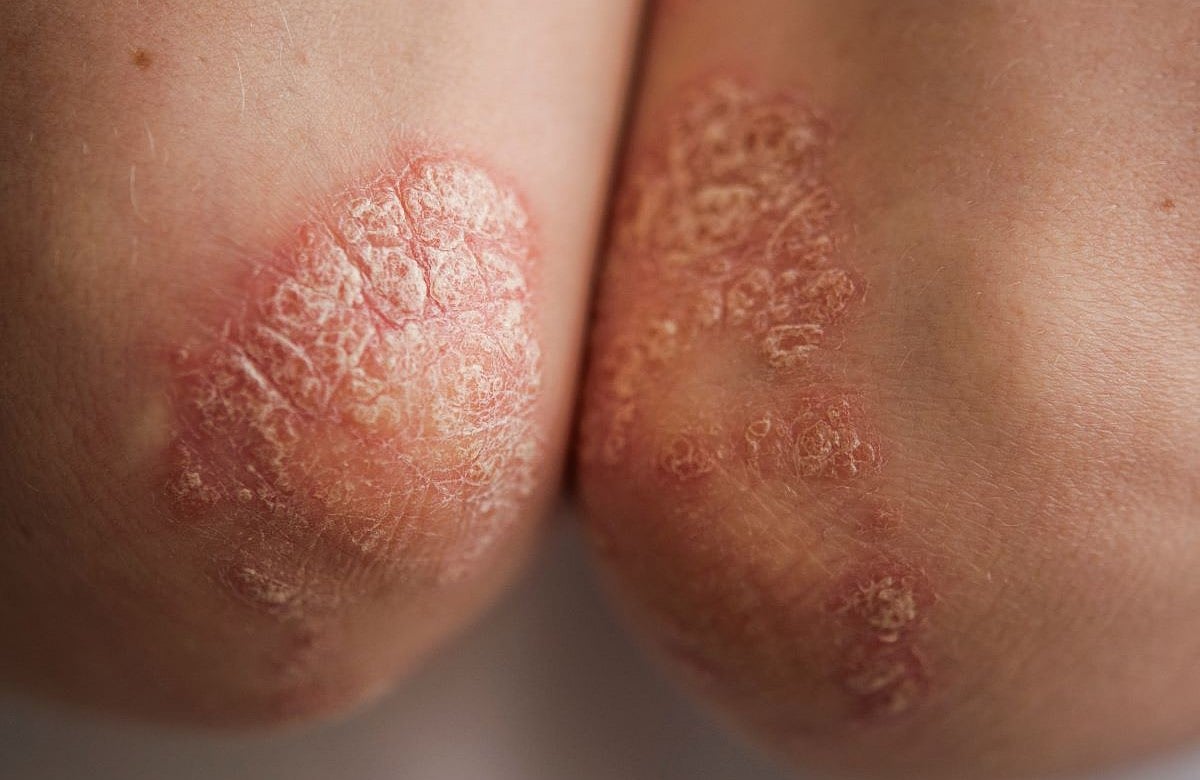
New Pill Could Change Plaque Psoriasis Treatment
Folks with severe plaque psoriasis often have to choose between convenient pills that don’t work very well or highly effective injections that come with the hassle of needles.
That trade-off may soon change. New clinical trial data suggests a once-daily pill called zasocitinib may provide the clear skin once only expected from shots....
- HealthDay Staff HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
Burnout Driving Family Doctors to Quit Medicine, Study Finds
You are more likely to lose your family doctor if they’re stressed and burned out, a new study reports.
Family doctors struggling with burnout are more likely to quit medicine altogether or leave their practice for a new one, researchers found.
Doctors were 70% more likely to leave medicine if they were feeling burned out, whic...
- Dennis Thompson HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
Researchers Explore When Crying Helps You
You might think shedding tears is a natural way to vent stress and reset the mind after a difficult day.
But new research suggests that a good cry isn’t the universal mood-booster we once thought it was.
An Austrian team took a closer look at what makes people cry, individual differences in crying and how it makes people ...
- Deanna Neff HealthDay Reporter
- |
- April 2, 2026
- |
- Página completa
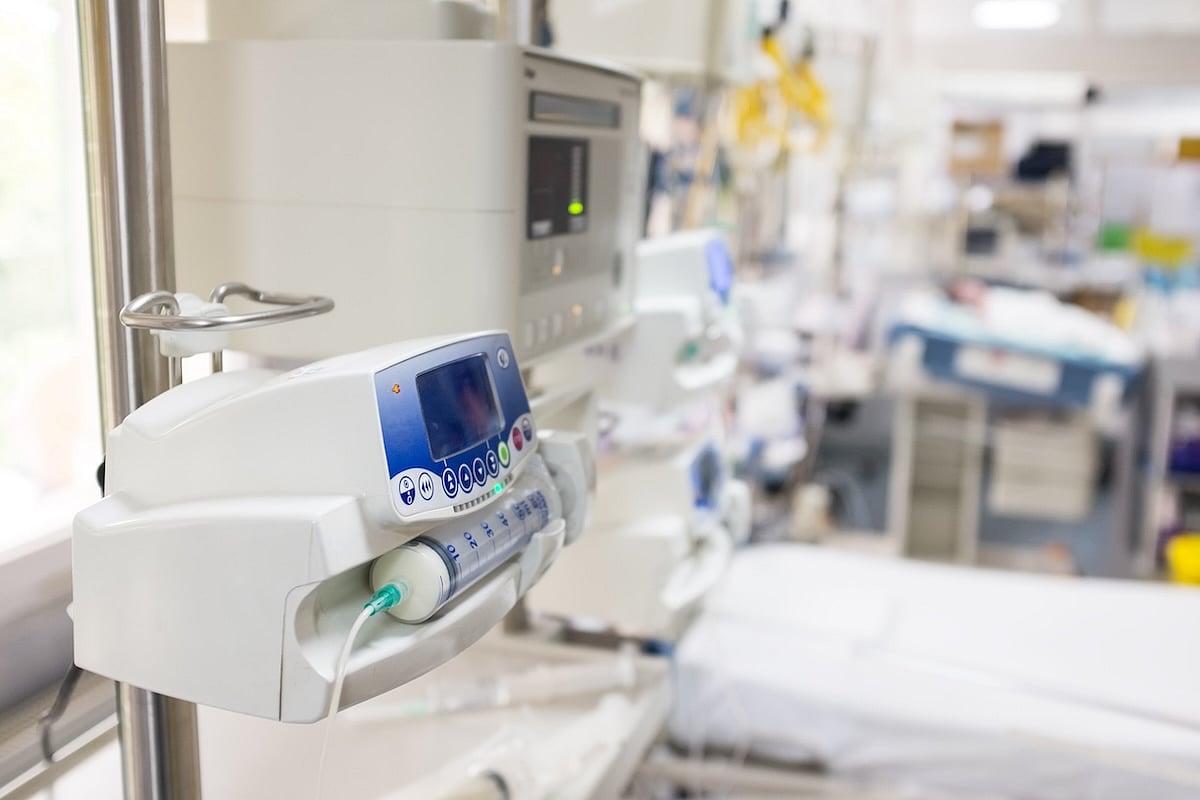
Hundreds of U.S. Hospitals at Risk of Shutting Down From Medicaid Cuts
A new analysis from Public Citizen found that 446 hospitals are at high risk of closing or cutting services due to planned Medicaid cuts under President Donald Trump.
The report looked at financial data from about 95% of U.S. hospitals between 2022 and 2024.
Medicaid plays a major role in hospital funding, covering about one-fifth of...
- HealthDay Staff HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Honey Almond Cream Cheese, Sold at Einstein Bros. Bagels, Recalled Due To Undeclared Nuts
A popular cream cheese spread sold at Einstein Bros. Bagels locations is being recalled due to a labeling mix-up that could put people with nut allergies at risk.
Schreiber Foods is recalling 144 cases of Honey Almond Cream Cheese Spread after noticing that some containers may contain almonds that are not clearly listed on the packaging, t...
- HealthDay Staff HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Trump Supports Surgeon General Pick Despite Senate Concerns
The White House is standing behind its pick for surgeon general, even as questions about her nomination continue.
President Donald Trump nominated Dr. Casey Means, but her confirmation has stalled after a tense U.S. Senate hearing earlier this year.
In a statement on Monday, press secretary Karoline Leavitt said the administration su...
- HealthDay Staff HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Supreme Court Blocks Colorado Limits on Therapy for LGBTQ Minors
The U.S. Supreme Court has blocked a Colorado law that forbid mental health professionals from trying to change LGBTQ minors’ sexual orientation.
In an 8-1 ruling, the court said the law violated free speech protections by limiting what therapists can say during sessions.
The case was brought by a Christian therapist who argued...
- HealthDay Staff HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Antidepressant Might Help Long COVID Fatigue, Study Says
A common antidepressant appears to help reduce fatigue in people living with long COVID, a new study says.
Fluvoxamine – a low-cost and widely available antidepressant – significantly improved fatigue among long COVID patients within two to three months, researchers reported March 31 in the Annals of Internal Medicine....
- Dennis Thompson HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Home-Delivered Groceries Boost Heart Health In Food Deserts, Study Says
Home-delivered groceries can help people who live in food deserts improve their heart health, a new study says.
Black adults experienced a significant reduction in both blood pressure and cholesterol after receiving home deliveries of groceries selected under the heart-friendly DASH diet, researchers reported at an American College o...
- Dennis Thompson HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Nicotine E-Cigarettes Help Smokers Quit, Review Concludes
E-cigarettes loaded with nicotine can help people quit smoking, a new evidence review has concluded.
Nicotine vapes produce quit rates 20% to 40% higher than traditional nicotine replacement therapies like patches or gum, researchers recently reported in the journal Addiction.
“We set out to determine if scientists agr...
- Dennis Thompson HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Kinesio Taping’s Benefits in Doubt, Major Evidence Review Finds
Elite athletes often show up at the starting line with legs, arms and shoulders covered in strips of brightly colored tape.
This “KT tape” – kinesio taping – is meant to ease muscle and joint pain and boost range of movement.
But KT tape might not be very effective at all, instead working mainly as a placebo f...
- Dennis Thompson HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
High Sodium Intake May Trigger New Heart Failure
Most folks know that too much salt can lead to high blood pressure, but new research suggests it may be even more dangerous than thought.
A Vanderbilt University team found that excessive sodium intake was a direct, independent trigger for new-onset heart failure among a high-risk population.
The research, recently published in the <...
- Deanna Neff HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa
Study Shows BMI Often Gets Your Weight Category Wrong
For decades, Body Mass Index (BMI) has been a standard tool doctors use to tell patients if they are underweight, normal weight or obese.
But a new study shows that this simple math equation — an estimate of based only on height and weight — is often wrong.
Research to be presented in May at the European Congress on...
- Deanna Neff HealthDay Reporter
- |
- April 1, 2026
- |
- Página completa